Obesity is recognized as one of today’s most serious public health problems. Worldwide an estimated 2 billion adults are overweight (BMI >25) , of whom 650 million are considered to be affected by obesity (BMI >30).That equates to 39% of adults aged 18 or over who are overweight, with 13% obese. 
The worldwide prevalence of obesity nearly tripled between 1975 and 2016. It is estimated that most of the world's population live in countries where excess weight and obesity kills more people than being underweight. If current trends continue, by 2025, 2.7 billion adults could be overweight, over 1 billion affected by obesity, and 177 million adults severely affected by obesity.
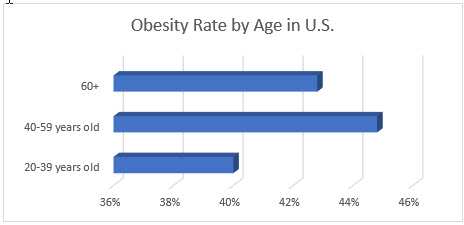
In the United States, obesity prevalence climbed from 30.5% in 1999-2000 to 42.4% in 2017-2018. Medical costs for persons with obesity in 2008 were estimated to add $147 billion to the country’s healthcare bill and obesity affects all age groups.
Sixteen states now have an adult obesity prevalence at or above 35 percent: Alabama, Arkansas, Delaware, Indiana, Iowa, Kansas, Kentucky, Louisiana, Michigan, Mississippi, Ohio, Oklahoma, South Carolina, Tennessee, Texas, and West Virginia. This is up from twelve states in 2019.
Obesity affects children too. According to the World Health Organization, an estimated 41 million children under the age of 5 years were overweight or obese in 2016. The prevalence of overweight and obesity among children and adolescents aged 5-19 rose dramatically, from just 4% in 1975 to over 18% in 2016. While just under 1% of children and adolescents aged 5-19 were obese in 1975, more than 124 million children and adolescents (6% of girls and 8% of boys) were obese in 2016. In the U.S., among children and adolescents aged 2-19, obesity affected 19.3%.
Health impact
Obesity can lead to adverse health consequences, including heart disease, stroke, type 2 diabetes and certain types of cancer. It reduces life expectancy by an average of three to 10 years. In Europe, obesity and being overweight are estimated to contribute to at least one in every 13 deaths. Day-to-day problems include breathlessness, increased sweating, snoring, difficulty doing physical activity, and joint and back pain. It can affect relationships with family and friends, and may lead to depression.
Children who have obesity are more likely to become adults with obesity. What’s more, if children have obesity, their obesity and disease risk factors are likely to be more severe in adulthood. Childhood obesity is also related to psychological problems, such as anxiety and depression, low self-esteem and lower self-reported quality of life, and social problems, such as bullying and stigma.
Impact of COVID-19
The pandemic has exacerbated the issue. COVID-19 death rates are 10 times higher in countries where more than half of the adult population is classified as overweight. The country with the lowest COVID-19 death rate – Vietnam – has the second lowest level of population overweight (18.3%). In contrast, the country with the third highest COVID-19 death rate – the United Kingdom – has the fourth highest prevalence of overweight citizens at 63.7%. With 67.9% of the population overweight, the United States has the next highest death rate, at 152.49 deaths per 100 000.
Children who are overweight or obese have suffered during the pandemic as well. In the U.S., among a cohort of 432,302 persons aged 2–19 years, the rate of BMI increase doubled during the pandemic, probably due to COVID-19-related circumstances, such as loss of family income or remote learning, which in turn contributed to weight gain, stress, irregular mealtimes, less access to nutritious foods, increased screen time, and fewer opportunities for physical activity.
In a CDC study of COVID-19 cases in patients aged 18 years and younger, having obesity was associated with a 3.07 times higher risk of hospitalization and a 1.42 times higher risk of severe illness (intensive care unit admission, invasive mechanical ventilation or death) when hospitalized.
What do we do?
The UK’s National Health Service says the best ways to treat obesity include:
- Eating a balanced, calorie-controlled diet as recommended by a GP or weight loss management health professional (such as a dietitian)
- Joining a local weight loss group
- Taking up activities such as fast walking, jogging, swimming or tennis for 150 to 300 minutes a week
- Eating slowly and avoiding situations where you know you could be tempted to overeat.
Other useful strategies include setting realistic weight-loss goals, involving family and friends in your efforts, monitoring your progress (e.g., making regular notes about weight in a diary), and getting psychological help from a trained professional.
Not to be ignored are strategies to address the sociological factors contributing to obesity, including education levels and family income. Obesity prevalence decreased by level of education, according to the CDC’s 2020 data.
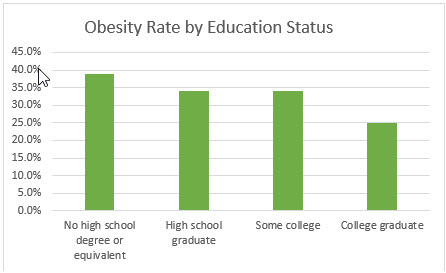
Among children and adolescents aged 2-19 in the United States, the prevalence of obesity decreased from 2011 to 2014 as the head of household’s level of education increased. Obesity prevalence was 18.9% among children and adolescents aged 2-19 years in the lowest income group, 19.9% among those in the middle-income group, and 10.9% among those in the highest income group.
Screening and testing
Given the potential health consequences of being overweight or obese, screening and testing should be part of the care plan. SEKISUI Diagnostics is a recognized leader in the development, manufacture and supply of innovative clinical chemistry reagents that enhance the clinical chemistry laboratory function, with over 1.8 billion tests performed each year. With more than 65 clinical chemistry assays, including cardiovascular, diabetes, renal, liver, therapeutic drug, and specialty assays, we can meet your individual needs.



Share Article